Why Cats Who Never Go Outside Still Need the Vet
Your cat may spend every day lounging in a sunny window or curled up on the couch. They’ve never roamed the neighborhood or tangled with a stray, so you might think that means they’re safe from illness. But here’s the truth: even cats who live strictly indoors still need regular cat wellness exams and up-to-date cat vaccinations.
Cats are experts at hiding pain and illness. As part of their survival instinct, they mask weakness, which means they can appear perfectly healthy while quietly developing serious conditions like kidney disease, dental problems, or diabetes. Skipping preventive care allows these problems to progress unnoticed until they become much harder, and more expensive, to treat.
And “indoor” doesn’t always mean “protected.” Illnesses and viruses can sneak into your home in surprising ways:
- Through open windows or screens when outdoor cats or wildlife wander nearby
- On shoes or clothing from people who’ve been around other animals
- From new pets joining the household
- During grooming appointments or boarding visits
That’s why veterinarians recommend at least one cat vet checkup every year, even for cats who never go outside. A yearly indoor cat health checkup gives your veterinarian the chance to spot small changes before they turn into bigger problems.
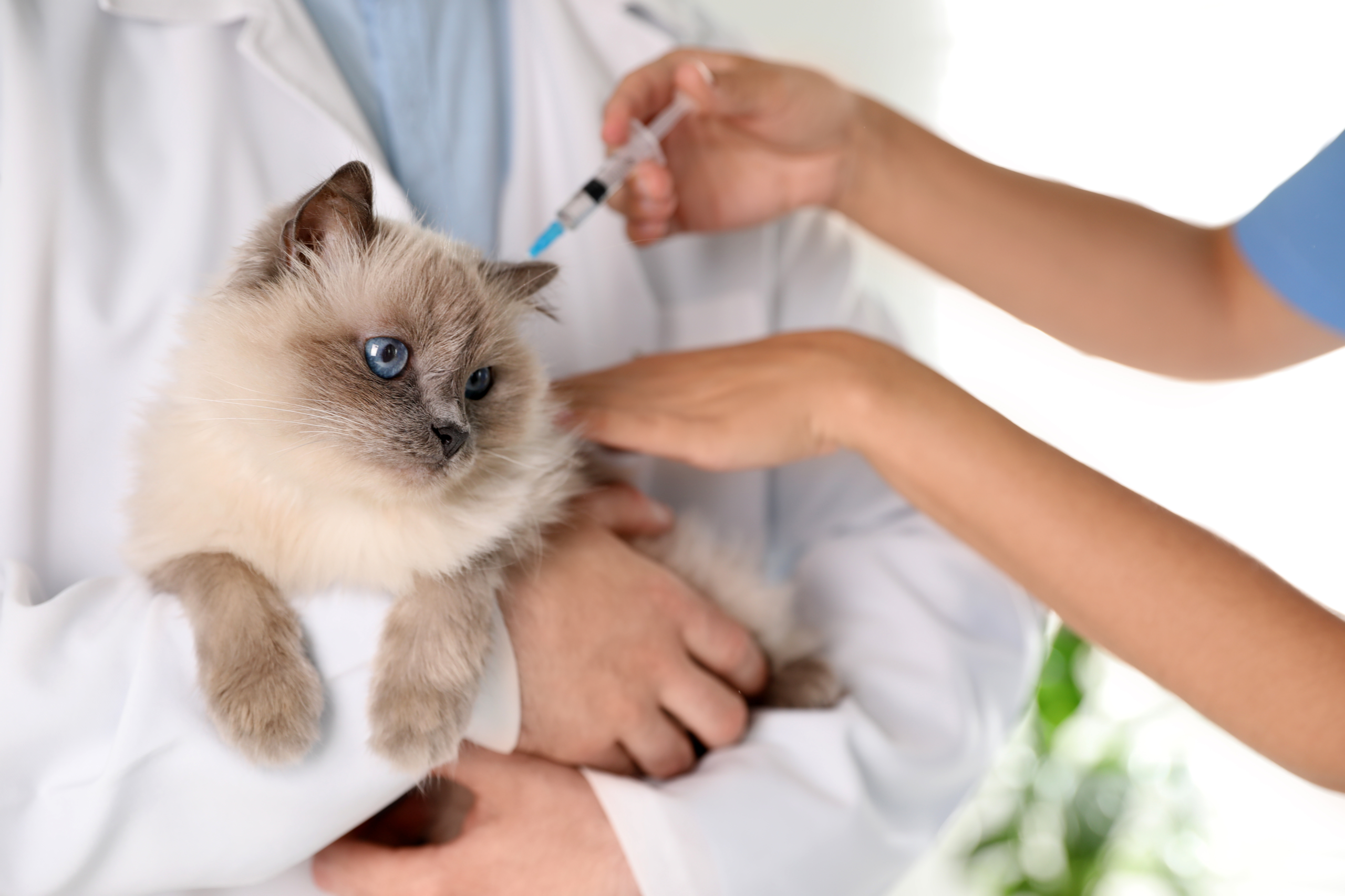
Vaccines Recommended for Indoor Cats
Just like humans, cats need vaccines to stay protected against dangerous diseases. Even if your cat never steps outside, vaccines provide a vital safety net against unexpected exposures.
Rabies Vaccine
- Legally required in most states
- Protects against a deadly disease that is 100% fatal once symptoms appear
- Rabies doesn’t always require outdoor exposure — bats, raccoons, or other wildlife can enter your home unnoticed
- Staying up to date on rabies vaccination for cats keeps your cat and your family safe
FVRCP Vaccine
This is a combination vaccine that protects against three highly contagious and serious feline illnesses:
- Feline Viral Rhinotracheitis – a severe upper respiratory infection
- Calicivirus – causes oral ulcers, respiratory illness, and can lead to chronic health issues
- Panleukopenia (feline distemper) – often fatal, especially in kittens
- Even if your cat never meets another animal, these viruses can be tracked indoors on clothing, shoes, or through other pets.
Other Vaccines
Depending on your cat’s health, age, and environment, your veterinarian may recommend additional vaccines. During a cat annual checkup, your vet will review your cat’s lifestyle and tailor vaccine recommendations accordingly.
The Role of Annual Wellness Exams
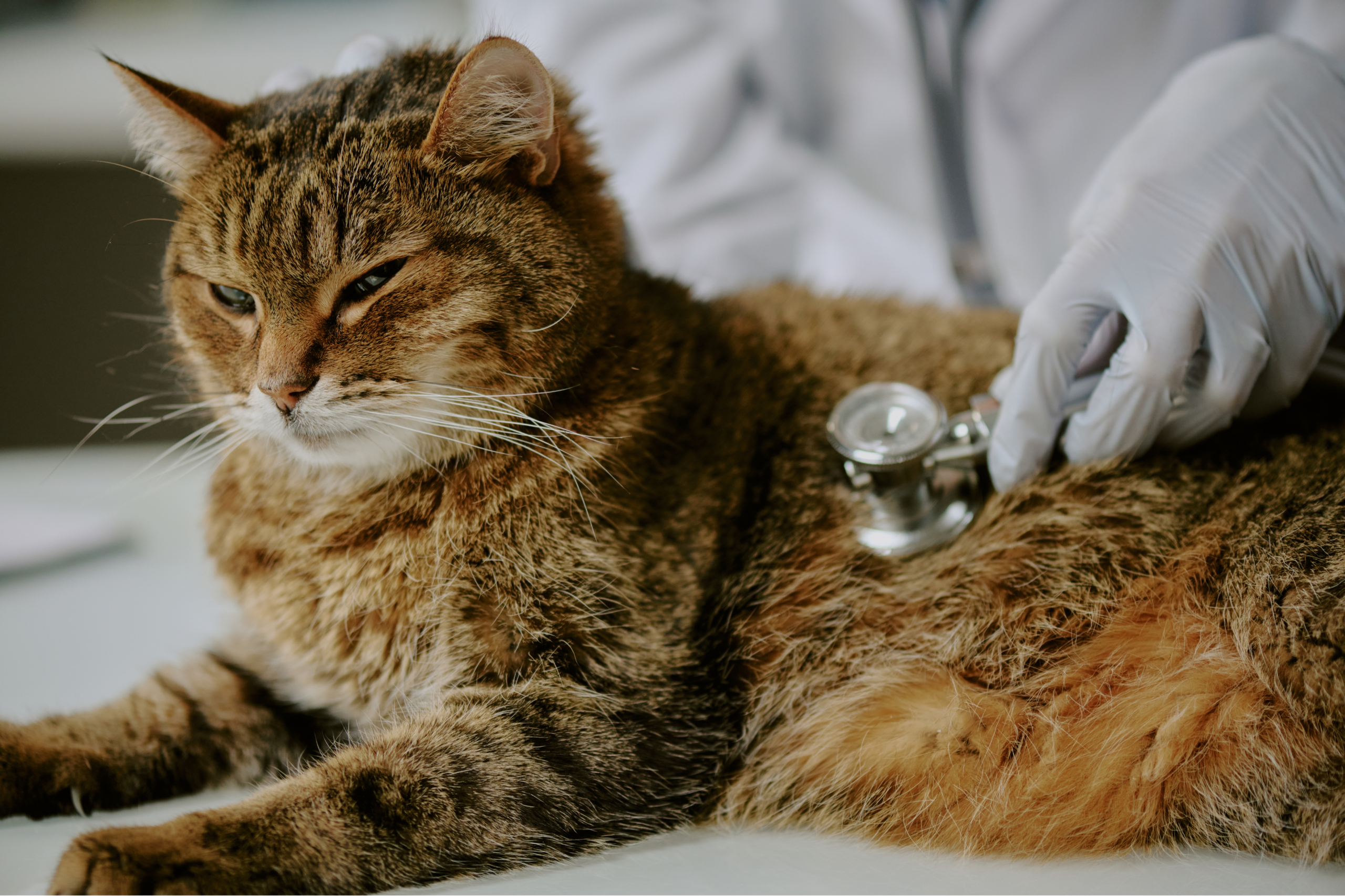
A cat wellness exam is about much more than vaccines. It’s a head-to-tail assessment that helps your veterinarian monitor your cat’s health over time and catch early warning signs.
At a typical cat vet checkup, your veterinarian may:
- Check weight and body condition to detect obesity or muscle loss early
- Inspect teeth and gums for dental disease, which can affect the heart and kidneys if untreated
- Run bloodwork to screen for conditions such as kidney disease, liver problems, or thyroid imbalances
- Examine eyes, ears, and coat for changes that could indicate underlying illness
- Discuss your cat’s nutrition, hydration, and behavior patterns
- Address small concerns (like vomiting hairballs more often or using the litter box differently) before they become emergencies
Cats age faster than humans, which means skipping even one annual exam is like missing several years of your own physicals. Preventive care is the best way to ensure your indoor cat lives a longer, healthier life.
Signs Your Indoor Cat May Already Need a Vet Visit
Even with routine checkups, there may be times when your cat needs veterinary care sooner. Call your veterinarian if you notice:
- Changes in appetite or water intake
- Sudden weight loss or gain
- Litter box changes (accidents, straining, or going more/less often)
- Reduced grooming, greasy coat, or over-grooming a specific area
- Hiding more than usual or changes in personality
- Persistent sneezing, coughing, or nasal discharge
These signs don’t always mean something serious, but they do mean your cat should be seen for a cat health checkup to rule out illness.
Why Preventive Care Saves Money — and Stress
Some pet parents hesitate to schedule a cat annual checkup because they worry about cost or stress for their cat. But in reality, preventive care often saves money in the long run.
Catching problems early means:
- Shorter, simpler treatments
- Less pain and discomfort for your cat
- Lower veterinary costs compared to advanced illness care
- More options for managing chronic conditions if they’re detected early
For example, treating early-stage dental disease may only require a cleaning, while untreated disease could result in tooth extractions and even organ complications. Likewise, early detection of kidney disease gives your cat the best chance for a longer, more comfortable life.
When you think of wellness exams as an investment in both your cat’s health and your peace of mind, the value becomes clear.
Give Your Cat the Gift of Health — For Free
At Pieper Veterinary Hospitals, we believe every cat deserves access to preventive care. That’s why we’re offering a free first wellness exam for cats who haven’t been in for a while.
Schedule your appointment before September 30, and you’ll also be entered to win a LitterBot automatic litter box.
Your cat may never set foot outside, but that doesn’t mean they’re safe from illness. The best time to protect your cat’s health is before something goes wrong. Book a cat vet checkup today and give your indoor cat the protection they deserve.